Pre-implantation Genetic Testing for Chromosomal Structural Rearrangements (PGT-SR)
What is PGT and PGT-SR?
Pre-implantation Genetic Testing (PGT), previously known as Pre-implantation Genetic Diagnosis (PGD), is a technique used alongside IVF by couples who have a particular inherited condition to avoid passing it on to their children. Pre-implantation Genetic Testing for Chromosomal Structural Rearrangements (PGT-SR) is used when either one of the couple is known to have a chromosomal structural abnormality. The technique allows embryos created through IVF to be tested in order to find out if they have inherited the chromosomal abnormality so that an unaffected embryo can be transferred to the womb and hopefully will result in the birth of an unaffected baby.
What is a chromosomal rearrangement?
A chromosomal rearrangement is a type of chromosomal abnormality involving a change in the structure of the native chromosome(s), which can be translocations, inversions or other complex changes. These events are caused by two breakages in one or two chromosome(s), followed by an exchange and then a rejoining of the broken ends to produce a new chromosomal arrangement.
Balanced Reciprocal Translocation
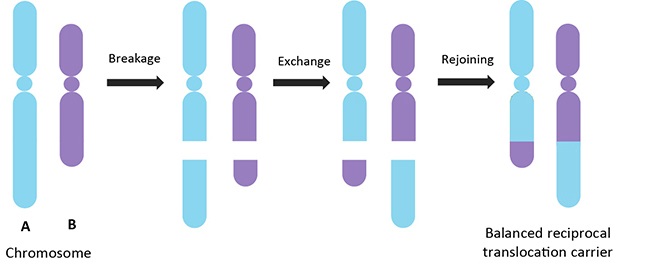
Robertsonian Translocation
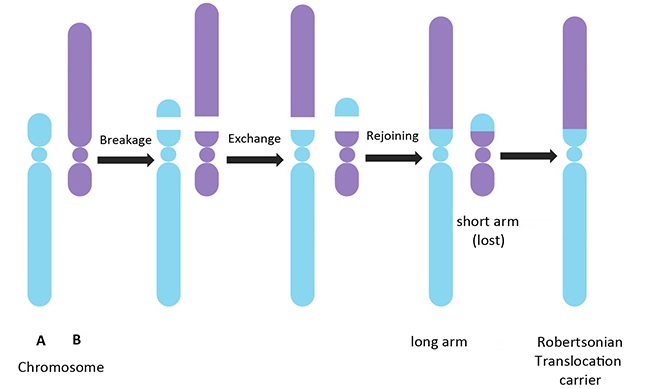
Inversion
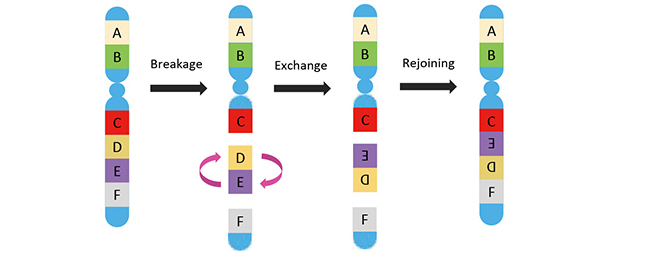
 scroll right to see more
scroll right to see more
Carriers of these chromosomal rearrangements are usually healthy, but they may produce sperm or eggs and hence subsequently embryos with an incorrect number of the whole or a segment of the chromosomes, i.e. unbalanced chromosomal translocations.
Balanced Reciprocal Translocation Gene map
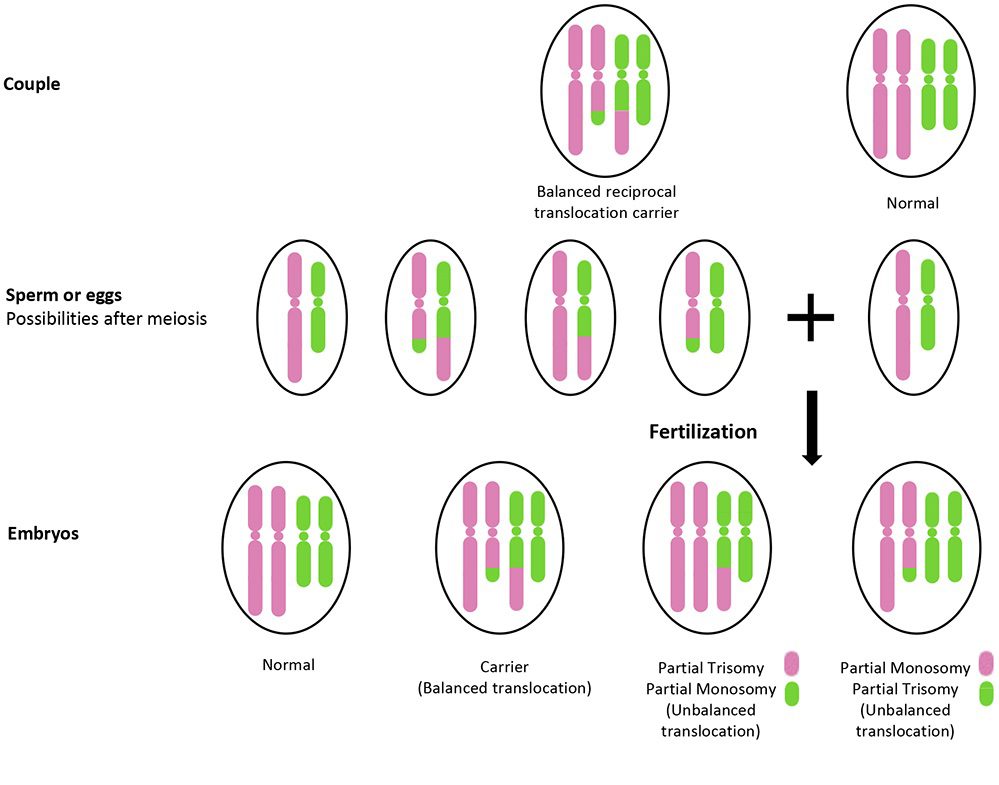
 scroll right to see more
scroll right to see more
Robertsonian Translocation Gene map
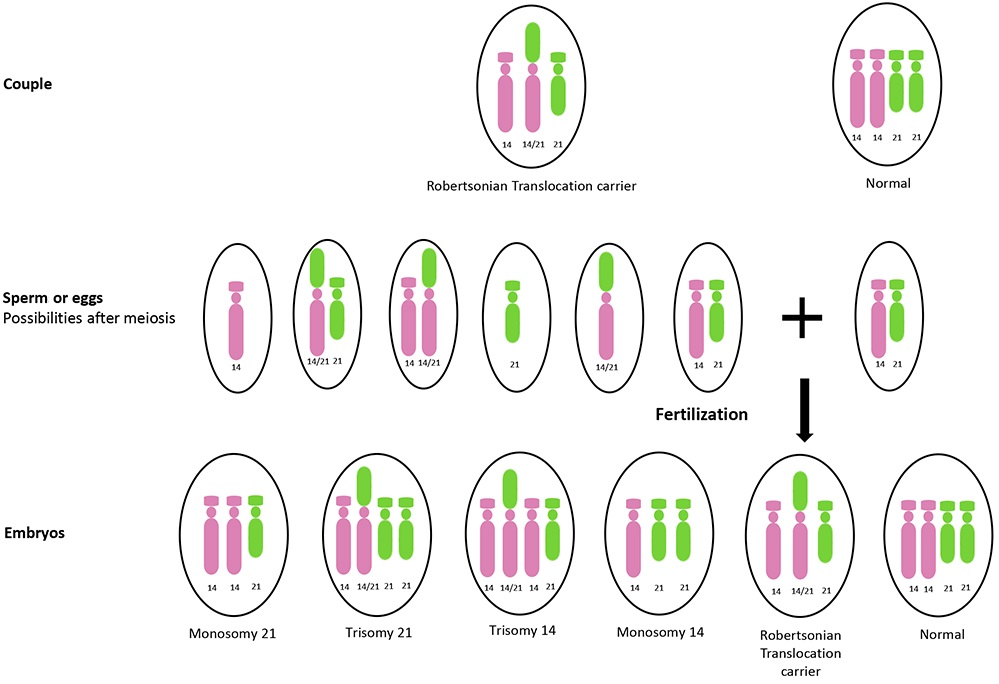
 scroll right to see more
scroll right to see more
Embryos with unbalanced translocations may grow at a normal rate in their early stages and look like the same as normal embryos. It is therefore possible to select an embryo for transfer that looks normal but actually contains an unbalanced translocation. This embryo will most likely fail to implant in the womb or miscarry during early pregnancy. However, sometimes a pregnancy can reach full term and an unhealthy baby is born with an unbalanced chromosomal translocation. PGT-SR can be used to check if an embryo has an unbalanced translocation so as to avoid transferring this embryo. Sometimes it is even possible to distinguish a normal embryo from an embryo with a balanced translocation. An embryo with a balanced translocation contains the correct number of genetic materials. It can grow to become a healthy person but will have the same problem that his / her parents are now facing when he / she plans to start his / her family. Therefore, if there is no normal embryo available, transferring an embryo with a balanced translocation can be considered.
What does PGT-SR involve?
PGT-SR Schematic Diagram
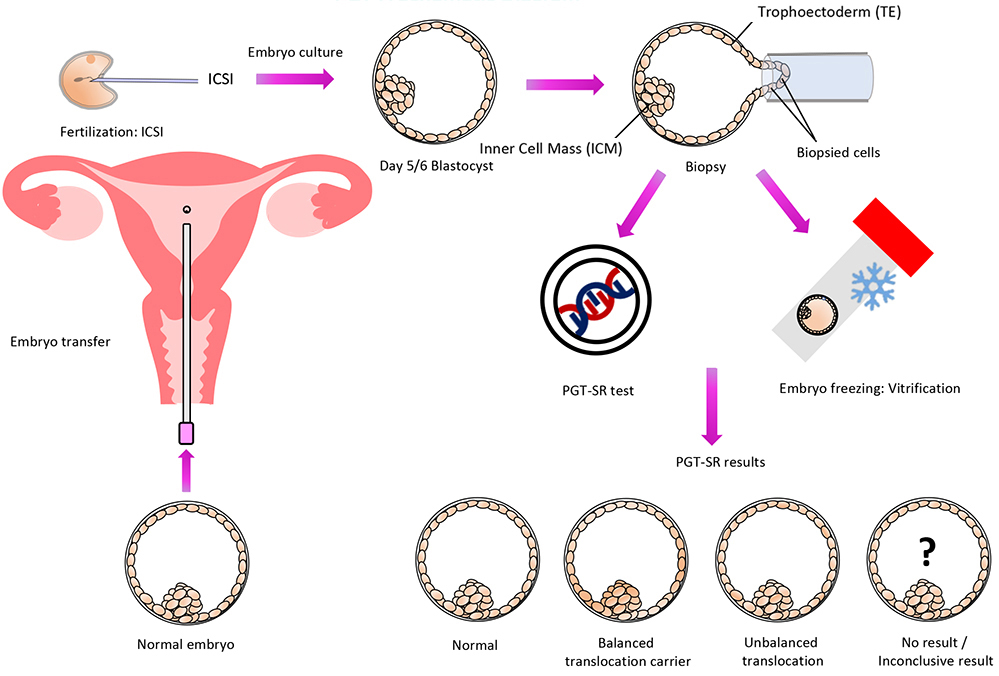
 scroll right to see more
scroll right to see more
The first step of PGT-SR is to go through an IVF treatment cycle. During the IVF cycle, each egg is fertilized with a sperm using intracytoplasmic sperm injection (ICSI) to avoid redundant sperm sticking to the outer sheath of the egg which will interfere with the test result. The embryos are cultured for five days, or sometimes six days, until they become blastocysts. Those embryos that can grow to become good quality blastocysts are biopsied whereby a few trophoectoderm (TE) cells are removed from the blastocyst. These cells are “extra-embryonic” and will produce tissues such as the placenta.
The inner cell mass (ICM) is the group of cells that will become the baby. There are over 100 trophoectoderm cells in a blastocyst so the removal of a few of these cells will have minimal impact on the embryo. Straight after the biopsy procedure the embryos are frozen to await the result of the test. The cells removed by biopsy are analyzed at the PGT laboratory. Frozen-thawed embryo transfer (FET) can be arranged in the following cycle if there are suitable embryos for transfer.
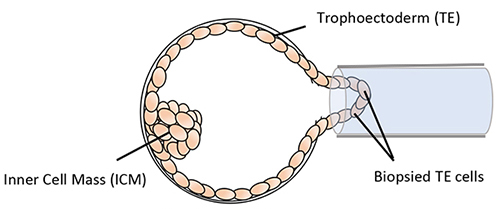
Blastocyst Biopsy
Does a couple with a known chromosomal structural abnormality have any alternatives to PGT-SR?
If the couple does not have fertility problems, they can choose to conceive naturally and then consider prenatal testing by chorionic villous sampling or amniocentesis. For most couples this route actually gives them the highest chance of having a healthy baby. However, it does mean that the couple may be faced with the very difficult decision about whether to continue or to terminate an affected pregnancy. Some couples consider other options including use of donor eggs, sperm donation, embryo donation adoption, or not having children.
Can PGT-SR exclude all other chromosome or genetic diseases?
PGT-SR tests for a specific chromosomal rearrangement only. It does NOT test whether the embryo has a correct number of chromosomes. The risk of having an embryo affected by a chromosomal aneuploidy (extra or missing chromosomes) is influenced by the age of the woman. The older the woman is, the higher the chance of having a pregnancy with an incorrect number of chromosomes. An aneuploid embryo will fail to implant mostly, or miscarry in early pregnancy. Occasionally, it may grow to term and may result in a baby with birth defects. Pre-implantation Genetic Testing for Aneuploidies (PGT-A) is a test to check if the embryo has a correct number of chromosomes. It is possible to perform both PGT-SR and PGT-A tests simultaneously with the same biopsied cells.
PGT-SR does NOT screen for and CANNOT detect any genetic disorders such as Thalassaemia. If either one or both partners carry a specific genetic disorder that could impair the normal development of a child affected by the disorder, the couple should consider Pre-implantation Genetic Testing for Monogenic / Single Gene Disorders (PGT-M).